Are you a risk-aware (neutral decision maker) or a risk-averse EBME manager?
When considering maintenance applications, EBME managers often face complicated decisions. These complications increase when they have to reflect on conflicting objectives such as clinical need, technical resources, cost, risk, and customer expectations. Maintenance work should consider repairable systems subject to random failures and analyse trade-offs between the costs and the benefits of the maintenance activities.
 This article aims to assist with decision making on planning maintenance for electro-medical devices that are in everyday use. The development of a decision maintenance strategy for these devices could lead to improved efficiency and use of staff time. Devices can be analysed from a risk point of view, to decide how often, if ever, regular planned preventive maintenance is actually required.
This article aims to assist with decision making on planning maintenance for electro-medical devices that are in everyday use. The development of a decision maintenance strategy for these devices could lead to improved efficiency and use of staff time. Devices can be analysed from a risk point of view, to decide how often, if ever, regular planned preventive maintenance is actually required.
The risk decisions of the EBME manager are very important and need to be pragmatic. We have limited budgets and resources. Some EBME departments 'over maintain' equipment. There are still EBME staff routinely stripping down equipment and carrying out unnecessary testing.
This dates back to the 1970's when most medical equipment was of analogue design, with circuits that were likely to drift out of tolerance due to the nature of the component used and the circuit designs.
Through the 80's there was a digital revolution in medical technology and that has continued through to current times, with tolerances becoming ever tighter, and product reliability constantly increasing.
To Maintain Or Not to Maintain?
There is little question that some equipment requires some sort of periodic routine maintenance. The reason for maintenance is simply that replacements are costly and each piece of equipment has a varied life expectancy. If not maintained there may also be a risk to patients. There are questions that we should answer, such as
1. Does the service manual specify that a service in necessary or recommended?
- If necessary, it must be done.
- If recommended it can be assessed for need and risk.
2. What is the likelihood that the risk will happen? (Think about why we test).
- If we test for electrical integrity, is there a risk that the electrical integrity of the device will fail making the device unsafe? Is there any need to electrically safety test double insulated equipment or is a physical inspection sufficient?
- If we test for calibration, is there an actual risk associated with calibration drift that will make the device fail or become unsafe?

When making sensible decisions, we must also look at the complete picture.
This will include the impact on:
- Clinical services,
- Technical performance,
- Scheduled activity,
- and cost.
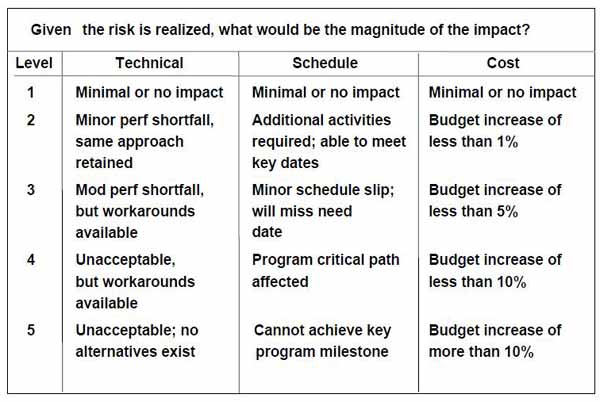
Given the risk is realised, will it really have an impact? How will that impact manifest itself. Will patients die, will costs rise, will the PPM schedule slip or...
- Is the likelyhood that patients will not die, cost and the PPM schedule will be unaffected?
There are many different types of equipment in use within the hospital, but many of these can be put into technology groups related to the clinical use of the equipment.
For example, an electrocardiograph (ECG) is used for monitoring the activity of the heart and is one type of technology group. There can be many ECG machines, of different makes, models, and age, in use that are all fulfilling the same functionality.
The basic example below does not give an extensive set of questions. Each technology group must be reviewed separately with questions based on that device. So when asking 'Does a ventilator need a planned inspection or should it be breakdown only' in this example, we come out with an impact score of 42. What does that number mean? It only has meaning if a risk assessment is carried out on a range of devices. Then a measurement scale of risk will become apparent.
It may be that based on available resources clinical risk and cost, the manager must specify that all equipment with a score above a specific score (e.g. 30) must have planned preventive maintenance inspections or full service carried out at regular intervals.
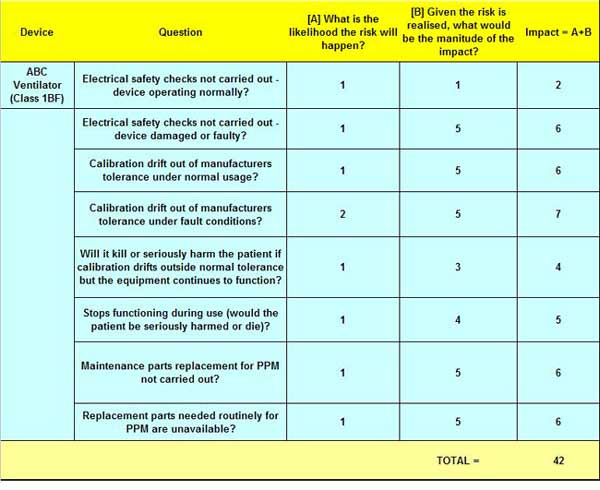
Therefore, on this device, regular or routine maintenance is required and this will keep the ventilator running smoothly until it eventually becomes obsolete. It also reduces the risk of a patient being harmed or killed through equipment failure.
However, every once in a while someone will ask, "Why maintain a piece of equipment that is relatively inexpensive to replace?" For example, a simple ward based electronic automatic blood ure machine. In the example below, the BP machine comes out with an impact score of 20. As our scale for planned inspections indicates that only devices over 30 would be put on the schedule, these blood pressure devices would be left off the PM schedule and be repaired only when reported.

Although there is not an easy answer to this question, both sides of the issue should be closely examined before any final decision is reached on whether or not a specific piece of equipment should or should not be maintained. All too often the answer to this question is based on a financial analysis, and not on a philosophy of equipment reliability and clinical risk.
In situations where a piece of equipment is inexpensive, the need for maintenance is often ignored and the device is operated until it fails. From a financial standpoint this might seem to be the best approach because of the savings in maintenance, labour and repair parts. Additionally, it eliminates placing the item on the maintenance schedule and the associated record keeping functions that go along with it. However, is the shortened life and early replacement really a cost-effective procedure?
Cost/Maintenance Ratio
The cost/maintenance ratio benefit can be determined easily by plotting the purchase and maintenance costs against the equipment life expectancy. Suppose the original equipment cost was £1500.00 and had a life expectancy of three years with no maintenance. If the estimated annual maintenance cost was £300.00 and would at least double the life of the unit, then the cost of maintenance can be justified because it eliminates the three-year replacement costs. However, there are two financial items that have not been taken into account in this analogy. One is the cost of the actual changing of the unit (labour). The second is the depreciation value of the equipment. Many managers do not consider depreciation, but it is a financial consideration. There also has been no anticipated increase in the equipment purchase price.
Real Costs
On the other side of the financial coin is the question of how much cost is really involved to replace the item. What happens if the equipment fails in the middle of the night or on the weekend and a replacement is not available or someone is not around to change it. There also are questions about what effect the failed item has on the patient process and at what cost. If the failure upsets the patient process flow and requires changes or adjustments to other elements of diagnostic or therapeutic care (that are non-automatic), then additional labour costs out of the norm will be incurred. (Perhaps in other budgetary areas outside the EBME managers responsibility) When considering the operating reliability and life of a piece of equipment, the cost of maintenance becomes a secondary issue. More important is the reliable operation of the patient care and process (Pathway), and the extended operating life of the item. By maintaining the equipment in good operating condition, the reliability of the patient pathway remains at peak performance. Additionally, properly maintaining the equipment not only extends its operating life (along with the reduced replacement cost), but its anticipated 'end of life' failure / obsolescence can be estimated. Being able to predetermine this date allows a Hospital the flexibility of replacing the item when it is the most advantageous and the least disruptive to the Hospital operations. This includes the proper purchasing and receipt of the item as well as the scheduling of the repair personnel. Our position is to maintain equipment as part of a planned system. Properly maintaining the equipment tells the owners (private or public) that your operational management is responsible and organized. On the other hand, if you ignore planned preventive maintenance on some items and stress it on others, you are sending mixed signals to the people responsible for maintenance, telling them that maintenance can be ignored if they have other things to do. Keeping the proper focus on maintenance keeps the proper focus for the entire Hospital operation.
Reliability Centred Maintenance (RCM)
Reliability Centred Maintenance can also be used to create a cost-effective maintenance strategy to address dominant causes of equipment failure. It is a systematic approach to defining a routine maintenance program composed of cost-effective tasks that preserve important functions. The important functions (of a piece of equipment) to preserve with routine maintenance are identified, their dominant failure modes and causes determined and the consequences of failure ascertained. Levels of criticality are assigned to the consequences of failure. Some functions are not critical and are left to "run to failure" while other functions must be preserved at all cost. Maintenance tasks are selected that address the dominant failure causes. This process can only address maintenance preventable failures, i.e. it cannot defend against unlikely events, non-predictable acts of nature, etc. The result is a maintenance program that focuses scarce economic resources on those items that would cause the most disruption if they were to fail. RCM emphasises the use of Predictive maintenance (PdM) techniques in addition to traditional preventive measures.
Sources:
http://www.wwdmag.com/To-Maintain-Or-Not-to-Maintain-article1736
http://www.emeraldinsight.com/Insight/viewContentItem.do?contentType=Article&contentId=1505911 (Link no longer functional).
http://bmf.hu/conferences/SAMI2003/MADARASZ.pdf
https://www.ebme.co.uk/articles/management/reliability-centred-maintenance-rcm
John Sandham IEng MIHEEM MIET



