Using vacuum assisted closure
Introduction
 Vacuum assisted closure (also called vacuum therapy, vacuum sealing or topical negative pressure therapy) is a sophisticated development of a standard surgical procedure, the use of vacuum assisted drainage to remove blood or serous fluid from a wound or operation site.
Vacuum assisted closure (also called vacuum therapy, vacuum sealing or topical negative pressure therapy) is a sophisticated development of a standard surgical procedure, the use of vacuum assisted drainage to remove blood or serous fluid from a wound or operation site.
The application of controlled levels of negative pressure has been shown to accelerate debridement (The process of cleaning an open wound by removal of foreign material and dead tissue, so that healing may occur without hindrance.) and promote healing in many different types of wounds. The optimum level of negative pressure appears to be around 125 mmHg below ambient and there is evidence that this is most effective if applied in a cyclical fashion of five minutes on and two minutes off.
It is believed that the negative pressure assists with removal of interstitial fluid, decreasing localised oedema and increasing blood flow. This in turn decreases tissue bacterial levels. Additionally, mechanical deformation of cells is thought to result in protein and matrix molecule synthesis, which increases the rate of cell proliferation. Despite the significant costs involved, the technique is said to compare favourably in financial terms with conventional treatments in the management of difficult to heal wounds.
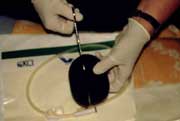 In essence the technique is very simple. A piece of foam with an open-cell structure is introduced into the wound and a wound drain with lateral perforations is laid on top of it. The entire area is then covered with a transparent adhesive membrane, which is firmly secured to the healthy skin around the wound margin. When the exposed end of the drain tube is connected to a vacuum source, fluid is drawn from the wound through the foam into a reservoir for subsequent disposal.
In essence the technique is very simple. A piece of foam with an open-cell structure is introduced into the wound and a wound drain with lateral perforations is laid on top of it. The entire area is then covered with a transparent adhesive membrane, which is firmly secured to the healthy skin around the wound margin. When the exposed end of the drain tube is connected to a vacuum source, fluid is drawn from the wound through the foam into a reservoir for subsequent disposal.
The plastic membrane prevents the ingress of air and allows a partial vacuum to form within the wound, reducing its volume and facilitating the removal of fluid. The foam ensures that the entire surface area of the wound is uniformly exposed to this negative pressure effect, prevents occlusion of the perforations in the drain by contact with the base or edges of the wound, and eliminates the theoretical possibility of localised areas of high pressure and resultant tissue necrosis.
In the early studies, negative pressure within the wound was achieved by the use of conventional methods such as wall suction apparatus or surgical vacuum bottles. Both these systems are associated with practical problems in terms of the delivery, control and maintenance of the required levels of negative pressure.
In 1995, a commercial system for promoting vacuum assisted closure (VAC) was introduced into the United States market. This equipment, called the VAC, was designed to overcome some of the previous problems. The heart of the system is a microprocessor-controlled vacuum unit that is capable of providing controlled levels of continuous or intermittent sub-atmospheric pressure ranging from 25 to 200 mmHg.
Two types of unit are available, a mains operated system with a canister volume of 300 ml for patients with limited mobility or very heavily exuding wounds, and a lightweight, battery-powered unit with a canister volume of 50 ml that can deliver therapy to an ambulatory patient with minimal to moderate levels of exudate (Liquid containing proteins and white cells). This system has a battery life of about 17 hours. The large system is fitted with various audible and visual alarms to indicate if the unit is tipped greater than 45 degrees, the canister is full, or the dressing has an air leak.
Negative pressure therapy is an "effective treatment modality for a variety of chronic wounds" producing healing in certain types of pressure ulcers 61% faster than saline soaked gauze whilst reducing costs by 38%. However, further analysis is required comparing treatment costs of VAC with other conventional treatments in the UK.
Sources:
http://www.worldwidewounds.com/2001/may/Thomas/Vacuum-Assisted-Closure.html
http://www.kci1.com/products/vac/vacdressings/index.asp


