What is an infusion system?
An infusion system is the process by which an infusion device and any associated disposables are used to deliver fluids or drugs in solution to the patient by the intravenous, subcutaneous, epidural or enteral route.
The process comprises:-
Prescription of the fluid or drug;
Healthcare professional Clinicians judgement.
Preparation of the infusion solution;
Always in accordance with Manufacturers instructions/directions.
Selection of the appropriate infusion device;
None, Monitor, Controller, Syringe Driver/Pump, General-purpose/Volumetric Pump, PCA Pump, Ambulatory Pump.
Calculation and setting of the rate of infusion;
Many devices incorporate Dose Calculators to assist with patient weight/drug units and fluid delivery over time calculations.
Monitoring and recording of the actual delivery.
Modern infusion pumps (clever as they are!) require frequent monitoring to ensure that they are delivering the prescribed treatment. Free flow of fluid due to incorrect housing of pump insert or syringe is a common cause of severe over infusion.
Patient Circuits/ Infusion giving pathway Tubing length & diameter; Filters; Taps; Anti-Siphon and Free-Flow prevention Valves; Clamps; catheters all have to be selected/ matched to the infusion system.
Optimal infusion, is the ability to reliably deliver the prescribed drug dose/volume to the patient, at pressures which overcome all baseline and intermittent resistance, but cause no harm to the patient.
Ideally pumps would reliably measure fluid flow, detect the infusion pressure and the presence of air in the line close to the patient vessel being infused, none do!
Patient Circuits/ Infusion giving pathway
Resistance is any impediment to fluid flow. The greater the resistance in the IV circuit higher pressure is required to obtain the prescribed flow. The internal diameter and kinking potential of connecting tubing, cannula, needles, and patient vessel's (phlebitis) all cause additive resistance to infusion flow. This along with filters, sticky solutions and syringe/cassette stiction can accumulate to the extent that infusion pumps are required to accurately deliver prescribed drugs to patients. These pumps must be capable of delivering infusions at pressures of between 100 and 750mmHg ( 2 to 15psi) A small car's tyre pressure is 26 psi!
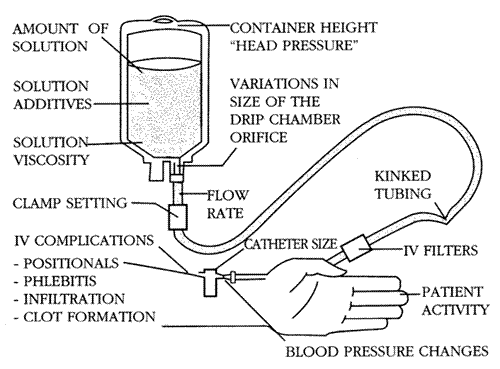
Gravity Drip Flow Manual IV System
The pressure available from a bag of saline = the height the bag is above the patient's heart.
If a saline bag is 68cm(27") above the patients heart the infusion pressure available is 50mmHg(1psi).
If the bag is twice that height above the patient 136cm (54") the available pressure is 100mmHg(2psi)
Pressure in context
If we are seeking to ensure that our IV infusion devices are compatible with pressures found in the patient's venous system then we need to be clear as to where in a range of pressures, the venous system lies. This will enable us to determine whether or not an IV pump pressure setting is going to be compatible with venous pressure at the IV site.
| Pressure mmHg | Example (rounded pressure values) | Pressure in psi |
| 2 - 20mm Hg | Central Venous pressure range | 0 - 0.4 psi |
| 10 - 30mm Hg | Peripheral Venous pressure range | 0.2 - 0.6 psi |
| 80-100mm Hg | Extravasation risk | > 2 psi |
| 100-150mm Hg | Systolic Arterial pressure range | 2 - 3 psi |
| 75mm Hg | Gravity pressure of fluid 100cm above cannulation site | 1.5 psi |
| 750mm Hg | Highest probable pressure required by an infusion pump | 15 psi |
| 1,000mm Hg | Many Ambulatory pump occlusion pressure settings | 20 psi |
What resistances does a pump have to overcome to deliver fluid?
To deliver simple electrolytes into an adult intravenous site through a 16G, 9 cm long cannula at 100 ml/h the pressures due to all the resistances can be summed as follows:-
| maximum adult venous pressure | 30 mm Hg |
| filter | 10 mm Hg |
| cannula | 100 mm Hg |
| administration set | 1mm Hg |
| Total = | 141 mm Hg |
Common types of hospitals infusion pumps
- General-Purpose / Volumetric
- Syringe Drivers
- Patient controlled analgesia (PCA)
- Ambulatory
In general
Infusion pumps use a positive pumping action, are powered items of equipment, which, together with an appropriate administration set, provide an accurate flow of fluids or drugs over a prescribed period. Volumetric pumps employ a linear peristaltic pumping mechanism or use a special cassette. Syringe pumps work by pushing the plunger of a disposable syringe along at a predetermined rate.
The type of pump used/selected will depend on the required volume, long & short-term accuracy and speed of infusion.
Many pumps operate from battery and mains electricity. They incorporate warnings and alarms of excessive upstream pressure, air in tube, syringe empty/ nearly empty and low battery. Normally the total volume of fluid to be delivered can be set, and following delivery an end of infusion, KVO (keep vein open) flow of 1 to 5 ml/hr will continue to infuse.
General-Purpose / Volumetric Pump
Utilise a linear peristaltic action or piston cassette pump insert to control the prescribed infusion volume. They are used to accurately administer intravascular drugs, fluids, whole blood and blood products. And can administer up to 1,000ml of fluid (normally from a bag or bottle) at flow rates of 0.1 to 1,000ml/hr.
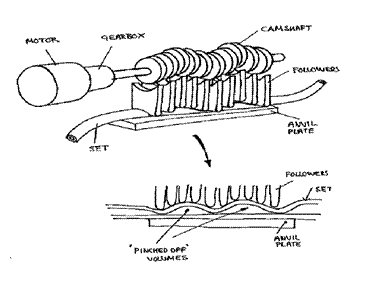
Most volumetric pumps will perform satisfactorily at rates down to 5ml/h. Although the controls can set rates below 1ml/h, these pumps are not considered appropriate for delivering drugs at such low rates.
Correct usage of administration sets
Most volumetric infusion pumps are designed for use with a specific type of infusion set. Therefore, the accuracy of delivery and of the occlusion pressure detection system depends partly on the set.
Some volumetric pumps use low cost standard infusion sets and it is important to note that each pump must be configured correctly for the specific set.
Sets that are incorrect, or not recommended, might appear to operate satisfactorily. But the consequences for performance, particularly accuracy, can be severe. For example,
- Under-infusion can result if the internal diameter is too small;
- Free-flow through the pump, over-infusion or leakage back into the bag or reservoir can result from tubing that is less flexible or has a larger outside diameter;
- Tubes can rupture if the construction materials are not sufficiently strong to withstand wear from the pumping action;
- Air-in-line and occlusion alarm mechanisms can be disabled through using the wrong set.
The action of the mechanism, which compresses and stretches the set during infusion, causes the set to wear out over time and this inevitably affects the accuracy of delivery. Recommended sets are designed in such a way that, except for large volume, high flow-rate infusions, wear and/or work hardening of the material will not adversely affect the accuracy.
Syringe Drivers
Utilise an electronically controlled, electric motor to drive the plastic syringe plunger, infusing the syringe contents into the patient. They effectively replace the Doctor or Nurses thumb by controlling the speed(flow rate), the distance (volume infused) and the force (infusion pressure) that the syringe plunger is pushed. The operator must use the correct make and size of syringe, ensure it is properly in place and frequently monitor that it's delivering the expected drug dosage. Syringe drivers administer up to 100ml of drug at flow rates of 0.1 to 100ml/hr.
These pumps are the preferred choice for lower volume and low flow rate infusions. Users should be aware that the flow delivered at the start of an infusion might be considerably less than the set value. At low flow rates the backlash (or mechanical slack) must be taken up before a steady flow rate is achieved. At low flows it can be some time before any fluid is delivered to the patient.

Patient controlled analgesia (PCA) Pump
Is a Syringe driver that allows the patient, within defined limits, to control their own drug delivery. They employ a patient hand control, which when pressed, delivers a pre-set bolus of analgesic drug. Immediately after delivery the pump will refuse to deliver another bolus until a pre-set time has passed. The pre-set bolus size and lockout time, along with background (constant drug infusion) are pre-programmed by the clinician.
Ambulatory (portable)
Small, light, battery powered syringe or cassette mechanisms. Many of the units in-use have only minimum alarms, therefore both patients and carers should be particularly vigilant in administration observations. Consideration also has to be given for the hazards a portable devices is exposed to e.g. knocks, fluids, electro-magnetic interference etc. In general critical drugs which require constancy of flow should not be administered using ambulatory pumps.
Therapy categories, Performance parameters and safety features
Pumps are designed for a variety of clinical applications and their performance characteristics will vary. The same level of technical performance of pumps is not necessary for every clinical therapy. The MHRA have divided therapies into three major categories according to the potential infusion risks to help purchasers and users select the pump(s) most appropriate to their needs.
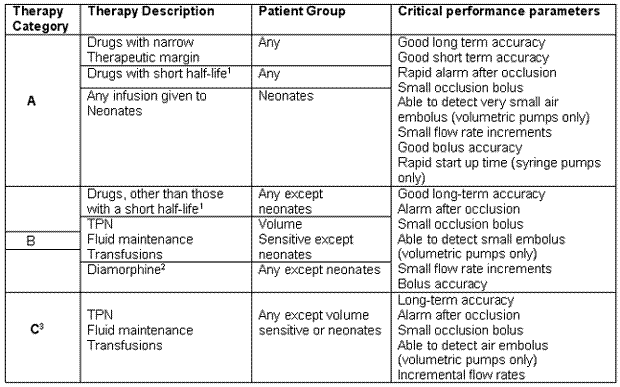
Decision tree for selecting the appropriate therapy category
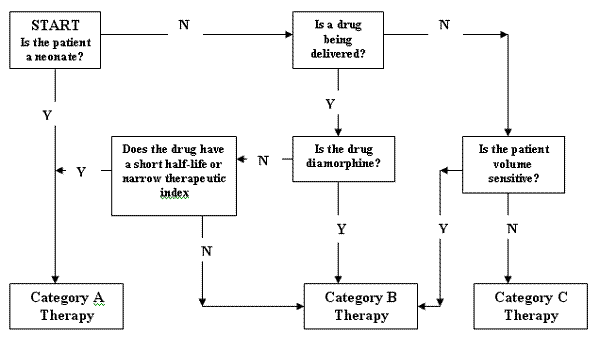
Choosing The Infusion Device
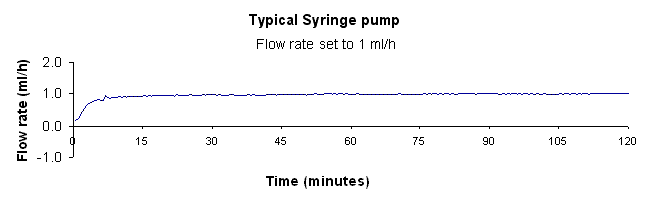
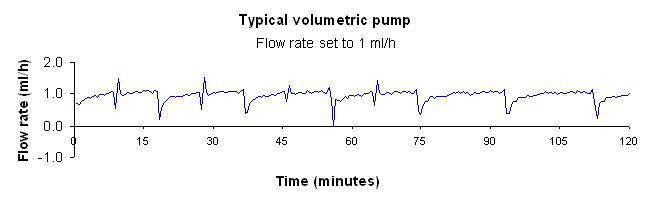
The pattern of delivery of fluid from an infusion pump is very dependent on the type of pump used.
These three graphs show typical flow patterns from a syringe pump, a volumetric pump and an ambulatory pump. Each of these pumps delivers fluid accurately (better than 5% of set rate) over long periods, but only the syringe pump delivers fluid accurately over very short periods (a few minutes).

Infusion pump associated hazards and problems
Tissuing
Infiltrations can occur at >100mm Hg(2 psi). Pumps delivering infusions at pressures of 750mm Hg (15 psi) to overcome fluid resistance are capable of producing extra-vascular infusion patient damage. Infusion pumps have adjustable pumping/Occlusion pressure settings (normally technical settings), newer units incorporate user settings.
The balance between setting the pumping pressure to overcome all baseline and intermittent resistance and prevention of tissuing is a major issue. Setting the pressure low, at best causes nuisance occlusion alarms. This becomes a major concern when a patient's blood pressure support depends on reliable drug infusion and the infusion is interrupted due to intermittent drug circuit resistance. Clinical advice is required to ascertain the appropriate setting for the patient.
What are the hazards caused to the patient by an:

Time to Alarm
Another factor relating to infusion pump pressure is the impact it can have on the time interval between when an occlusion occurs and the alarm sounds. The higher the pumps occlusion alarm/ pressure limit is set, the longer IV related problems have to develop before nursing staff are alerted by the alarm. Flow rate also affects alarm response time. Higher flow rates result in more rapid alarm response than lower flow rates.

Occlusion Bolus effect
Any blockage/occlusion of the giving pathway causes the upstream line pressure to increase to the pumps occlusion alarm/ pressure limit, which causes the tubing to expand/balloon. Clearing the occlusion e.g. opening the tap, roller clamp, kinked tubing will infuse a bolus into the patient. The higher the occlusion alarm/ pressure limit is set the larger the bolus.
Free-flow/siphonage
Although obvious to all, fully opening the roller clamp on a basic gravity infusion set-up will permit all the fluid and any air in the bag to infuse into the patient, we seem to abandon this basic logic when using a pump! If the pump is higher than 12 inches above the patient's heart, and the roller clamp is fully open, free-flow is likely occur if :-
- The tubing, syringe or cassette aren't carefully located into the housing.
- The pump door is opened or the syringe is removed from its' clamp.
- There is a break/leak in the upper part of the giving pathway or the syringe.
Air-in-line detection
International Standards require all General-Purpose pumps to have air embolus protection capable of detecting single bubbles of about 0.1ml. The ultrasonic air detection system in-use responds to any air in its' pathway. If the tubing is not pushed firmly into the detector slot or there are any small particles on the tubing or the detector it may respond with a false air-in-line alarm. Solutions prone to frothing will also activate the air sensor. Unexplainable false air-in-line alarms have been reported i.e. alarms for no apparent reason. This is at best a nuisance, and, when interrupting delivery of fast-acting, vasoactive drugs, can be hazardous! Further investigation of unexplained alarms is necessary.
Tampering
Staff must be aware that patients and visitors can open pump doors, remove syringes and administration sets, change settings and switch off pumps.
Faults
Genuine infusion pump malfunctions rarely occur, except when a pump has been dropped or damaged. Faulty batches of administration sets have caused problems. Prompt reporting of dropped pumps, suspect administration sets and unexplainable alarms will improve overall drug infusion safety.
Further Training
Practical training must be a pre-requisite for all staff and carers involved in the direct care of patients receiving parenteral nutrition or medication via infusion devices.
Additional training that is specific to the devices in use locally should be provided as part of local procedures.
If a new device is being introduced, whether purchased, borrowed or donated, training sessions should be arranged for all relevant staff before it is used
| When? | Ask yourself |
| Before use |
|
| Before pressing "start" |
|
| During the infusion at specified intervals |
|
| When an infusion system malfunctions |
|
| After use |
|
| When sending an infusion system to be repaired or serviced |
|
| When an infusion device has undergone service or repair |
|
| What to do when a serious adverse incident has occurred First take steps necessary for the well being of the patient and /or staff, then: |
|
| ALL medical devices can fail but an increasing number of incidents which result in significant morbidity or mortality arise out of user/device interface problems or because of poor practices. The aim of this new-sheet is to detail briefly some of the problems in an attempt to make users more aware of what can go wrong....it is all too easy to take equipment for granted. | |
Category "A" Therapy Infusion Pumps with associated deviation warnings |
|
| Based on Medical Device Agency (MDA) Device Bulletin Infusion Systems MDA DB2003 (02) Mar 03, and Evaluation 02110 | |
| All neonate infusion pumps require to conform to Therapy Category "A". | |
| Syringe pumps are the preferred choice for lower volume and low flow rate infusions. | |
| Volumetric pumps are the preferred choice for medium and high flow rate and large volume infusions. Most volumetric pumps will perform satisfactorily at rates down to 5 ml/h. |
|
| Therapy Category "A" Critical performance parameters:- Good long-term accuracy; Good short-term accuracy; Rapid alarm after occlusion; Small occlusion bolus; Able to detect very small air embolus (volumetric pumps only); Small flow rate increments; Good bolus accuracy; Rapid start-up time. |
|
| Important safety features in descending order of importance:- Anti-free flow device in administration set Free-flow clamp in pump when door opened Provision against accidental modification of settings Two distinct actions to change rate Two distinct and/or simultaneous actions to initiate bolus Syringe barrel clamp alarm, door open alarm or equivalent Syringe plunger disengagement alarm or equivalent Patient history log Volume infused display Technical history back-up Battery back-up |
|
| Deviation from "A" criteria: | Yellow card = Caution. | Red card = Warning. |
Syringe PumpsDeviations from "A" Category |
||
| Manufacturer & Model | Yellow Card | Red Card |
| Alaris Asena CC | Time to alarm on occlusion = 6min. | Constancy index at 1 ml/h = 13min. |
| Alaris Asena GS | Start-up time = 7 min. | |
| Arcomed SP6000 | Time to alarm on occlusion = 7.5min. Start-up time = 14.5min. |
Bolus accuracy = -24% |
| Braun Perfusor Compact S |
Occlusion bolus = 0.18ml Min occlusion alarm = 225mmHg No technical history log |
Time to alarm on occlusion = 30min. |
| Fresenius Vial DPS-IS | Start-up time = 11.5min No technical history log |
|
| Graseby Omnifuse | Time to alarm on occlusion = 7min. Start-up time = 11.5min. |
Bolus accuracy = -20.5% |
| Medex 3010 | Min occlusion alarm = 200mmHg Start-up time = 19min. |
Time to alarm on occlusion = 25min. |
Notes: Constancy index; The principle is that the constancy index of the pump should be less than or equal to the half-life of the drug used.
| Deviation from "A" criteria: | Yellow card = Caution. | Red card = Warning. |
General Purpose - Volumetric PumpsDeviations from "A" Category |
||
| Manufacturer & Model | Yellow Card | Red Card |
| Alaris Signature Pressure Mode |
Constancy index at 1 ml/h = 6min. | |
| Alaris Signature Resistance Mode |
Constancy index at 1 ml/h = 7.5min. | |
| Arcomed Vp5005 | Accuracy + 5.8% at 1 ml/h Constancy index at 1 ml/h = 8min. |
No Anti free-flow device in administration set |
| Baxter Colleague | Accuracy - 5.2% at 500 ml/h Constancy index at 1 ml/h = 7min Min occlusion alarm = 103 - 310mmHg |
|
| Braun Infusomat fms | Occlusion bolus = 0.23ml Min occlusion alarm = 300mmHg Air detection = 100ul |
Time to alarm on occlusion = 17min. Constancy index at 1 ml/h = 22.5min. |
| Graseby 500 | Time to alarm on occlusion = 8 min. | Bolus accuracy = -14% Constancy index at 1 ml/h = 19.5min. |
| Terumo TE172 | Constancy index at 1 ml/h = 3.5min. | No Anti free-flow device in administration set |
Notes: Constancy index; The principle is that the constancy index of the pump should be less than or equal to the half-life of the drug used.
Article by Mr. W O M Davis IEng FIIE