All strategic innovations require investment, and all investment requires approval. Make sure there is a strategic technology plan that underpins the organisations ‘Master Plan’. Technology is at the very core of NHS plans to deliver transformation and virtual warding, but making these big breakthroughs requires investment in medical equipment and IT infrastructure.
All strategic innovations require investment, and all investment requires approval. Make sure there is a strategic technology plan that underpins the organisations ‘Master Plan’. Technology is at the very core of NHS plans to deliver transformation and virtual warding, but making these big breakthroughs requires investment in medical equipment and IT infrastructure.
To deploy new technologies at scale, the NHS Trusts must have the right foundations in place, which include clinical engineering expertise. If the building blocks that make transformation possible are to be delivered, the technology strategy must include plans for both on and off-site activities. For this to work efficiently, it also requires IT connectivity between the different technologies.
This is a challenging strategy, and will require assessment, benefits analysis, and procurement committee approval. As part of the approval process, the financial mechanisms must also be decided. For example, should technology be bought from local revenue budgets, Trust Capital, leased, or some other mechanism, such as charitable funds? Only then, can the impact be achieved – delivering the innovations, improved clinical decision making, better patient outcomes, and improved organisational efficiency.

Through the smarter use of emerging technologies, the NHS can move services from generalised to personalised care delivery. As part of this, it is important to develop clearly understood strategies for buying products that can deliver the plan. All technology plans must be underpinned by standards to ensure that technology systems can talk to each other. New technologies can also help us to offer more dignified and independent care to people, in their own homes, keeping them out of hospital if they don’t need to be there. With an increasingly ageing population – where nearly one in 7 people is projected to be aged over 75 by 2040 – and more and more comorbidities, technology can do so much to help people to live independent lives and minimise the time they spend in clinical settings.

Remote monitoring played a crucial role during the pandemic and showed what could be achieved with the right plan, the right level of investment, and the right technological support. 18,000 people were monitored in their own homes during the covid pandemic, rather than being limited by the hospital ward capacity (bed shortages), and with the added risk of infection.
Norfolk and Norwich NHS Foundation Trust set up their virtual wards over a year ago. They managed to free up over 6,000 bed days for inpatients – and the initiative has patient satisfaction levels of 99%.

The NHS is planning to intensify the pace of the rollout of virtual wards so we can make sure that these services are available across the whole country.
The government has made £450 million available over the next 2 years to support this initiative.
The Future?
In the 1980’s, Asset management involved recording of the individual items within the healthcare organisation, and making sure it was serviceable, the main function being repair and maintenance.
In the last 20 years medical devices have become not only things you can touch, but also software components such as Health Level Seven or HL7, which refers to a set of international standards for transfer of clinical and administrative data between software applications used by various healthcare providers. Hospitals and other healthcare provider organisations typically have many different computer systems used for everything from billing records to patient tracking. All these systems should communicate with each other (or "interface") when they receive new information, or when they wish to retrieve information, but, at present, not all of them do. HL7 defines a series of electronic messages to support administrative, logistical, financial as well as clinical processes.
In the next 20 years, data in the electronic patient records or EPR will connect to software systems that use of complex algorithms and software, or in other words, artificial intelligence (AI), to emulate human cognition in the analysis, interpretation, and comprehension of complicated medical and healthcare data. Specifically, AI is the ability of computer algorithms to approximate conclusions without direct human input. The AI conclusions will be immediately available for clinician to review and enhance their own decisions about the clinical care provided to their patients. A typical system will have data being pushed directly from the healthcare technology into the Gateway management software, where it is processed for transmission to the electronic patient record. This is an instantaneous process with 100% accurate data entry. The data can then be used confidently for clinical decision support, clinical research, and finally into AI supported intelligent systems.
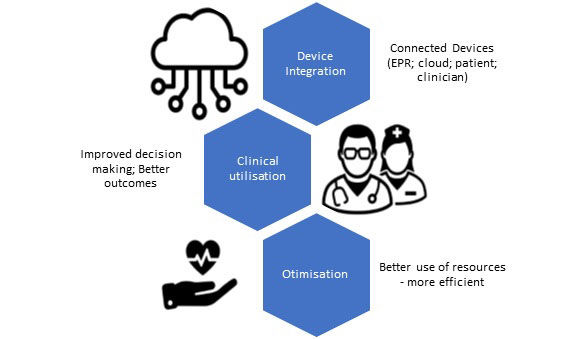
Organisations must understand the benefits of connectivity, only then can they deliver better patient outcomes, become more efficient, and deliver improved value.
https://www.nhsx.nhs.uk/key-tools-and-info/a-guide-to-setting-up-technology-enabled-virtual-wards/
https://www.england.nhs.uk/publication/2022-23-priorities-and-operational-planning-guidance/