Good morning everyone and thanks for inviting me to do this talk at the 10th EBME conference. That’s really exciting. It’s been really lovely to see some old faces and ex-colleagues, clients, and just generally I feel like the conference has got a real buzz about it so I’m delighted to be part of it.
Good morning everyone and thanks for inviting me to do this talk at the 10th EBME conference. That’s really exciting. It’s been really lovely to see some old faces and ex-colleagues, clients, and just generally I feel like the conference has got a real buzz about it so I’m delighted to be part of it.
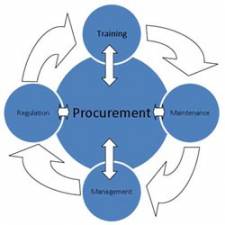
So, today, I am going to be talking about procurement and the transformation agenda, but I’m going to hopefully but a little bit of a different spin on it to perhaps what you would normally expect. So we know that procurement’s role is actually changing. So the first and hopefully obvious statement is that procurement is more than purchasing. So I think for many of us we’re very experienced with the transactional nature of procurement. I call it the tap-tap function - I think Mike Giles will probably be familiar with where that terminology comes from - and that is really around placing orders and all of the tasks that are necessary to do that. And that’s not what I’m going to talk about today. I’m going to talk about procurement more in terms of the transformation and where we need to be going for the future.
Hopefully many of you will recognise some of the stages of the procurement process and hopefully will be involved in most of those. But I’ve got a feeling that we’re not as involved as we should be. And I think that’s probably the key message that I’d like to get across during this presentation and perhaps in the discussion. I think rather than go through those stages, because some of them are very obvious, I think as you go towards the lower part of that slide you will actually recognise that you do get involved in helping to set up trials and evaluation and implementing new technology into use. And that’s generally, because let’s be honest, when you find out that something has arrived someone has to do something about it. And that’s not really good enough. So what we need to do is make sure that we’re in right at the beginning of the process, and the beginning of the process is about actually identifying what’s needed in the first place. And what’s needed in the first place is not necessarily what the clinician thinks they need, it’s not necessarily what the finance director thinks you need. So actually we need to put more intelligence into actually looking at what’s required in the very first place.
The end point of the procurement process should be getting either the right product, the right equipment, the right services, of course, in the right location and at the right time, and that’s obvious. But it’s just how do we actually achieve that? So I think before we go on to looking at how we can achieve that and what influence we can have, I’d just like to set the context. I think these are very challenging times, and we’ve heard a lot about that in the conference. We’ve heard about how technology, you know, an area where we’ve all get very significant interests, we’ve heard how that can actually influence the future.
So, just setting the context, we’re going through a very steep learning curve and transformation period, and that’s real. We’ve talked about it for quite a long time, but this is real now. This is getting serious. We need to do something different. There’s change taking place in terms of there’s more targets to meet. There’s more governance requirements. That puts actually an emphasis on the services that we provide as well. We need to invest more in equipment, not just replacement for what we have, but technology, real technology advancements that will actually help deliver some of this transformation.
Traditional methods, as we’ve heard and have discussed over the last couple of days, they’re just not keeping up with the financing requirement of actually investing in new technology or even replacing what we have. And we’ve touched slightly on that this morning with the managed equipment service. So I want to try and sort of look at that as well, the funding issues. We need to be more verbal or vocal about equipment replacement priorities. And I was really interested in Mike’s talk and looking at how Royal National Orthopaedic have actually identified their equipment replacement programmes. And I think that’s something that we can all learn from and that was a very good talk which hopefully you will take something away from.
The bottom point on that slide which I’ve just flicked to quickly was that the backlog equipment replacement in the NHS, and I actually talk primarily about NHS England actually, so apologies to Scottish and Irish colleagues, but the backlog is more than £1bn. The actual total medical equipment portfolio is I think around £4½-5bn. So a very significant asset, which we actually have a lot of involvement in what happens for the future. So I thought what would be really useful is actually to talk about the transformation agenda from an NHS perspective. And again apologies to Scottish and Irish colleagues, but we actually, I’ve looked more at the English acute sector market, which I think the majority of the audience are actually working within.
So there’s been quite a number of reports, reviews, all sorts of, I mean if you Google ‘transformation NHS funding’ you get thousands and thousands and thousands of entries. Most of them for management consultants I might add. So to transform something means to really change something. But the good old NHS, can we really change that, is it possible? Well I think it is possible, but it’s going to take a huge amount of effort. So all these reports I’d like to sort of, I mean there’s loads of them. There’s like Public Accounts committee, the King’s Fund, the NHS Confederation, I mean it just goes on and on. What I’ve tried to do here is pick out what I think are the very important documents, reviews that have been undertaken that actually really are influencing the transformation agenda. And that starts with the Lord Carter report.
I’m just going to do an ask the audience, a Who Wants to be a Millionaire moment, and that is how many of the audience have actually heard of the Lord Carter review? Good. That’s actually more than I necessarily expected. And that’s not because I’m giving you no respect. But it’s actually something that I think has been quite influential and probably does impact on our profession quite heavily. So that is the review of operational productivity and efficiency, primarily in the services delivered by the NHS and again England acute sector. And there’s been much reference to the report. So I’ve concluded that it must be worth discussing. So the final report was actually published in 2016, a think there was an interim version earlier, and the key themes around that were how do we actually improve efficiency and productivity? And it came up with 15 recommendations. You’ll be grateful to know I’m not actually going to go through all 15 recommendations, but there are some key themes and I think they’re actually worth mentioning.
So the report identified that there was significant and unwanted variation in costs across the NHS. So actually comparing different NHS hospitals and looking at the variations. And it concluded that there had to be a way of actually normalising some of those variations, and of course, as we know, the only way to really do that is to actually find out what good looks like in the first place. So I think it worked with, Lord Carter review did a review of a number of organisations including good organisations in their view to actually set some benchmarks, and out of that has come actually the model hospital. So, again, ask the audience, does everyone know about the model hospital? OK. So we’re diminishing in numbers now which is not unexpected because now we’re digging into the detail of what came out of the Lord Carter rather than the headline point.
So the model hospital, it looked at good practice in the NHS and elsewhere actually, not just the NHS, and it’s come up with a number of performance metrics. What we would know as KPIs. And priority has been given in think in the first instance to imaging and pathology. So every hospital now has actually had to submit their statistics which cover almost every aspect of the delivery of their service. So for imaging that’s their workforce, that’s how many scans they do, how long patients have to wait, I mean the list is endless. And there’s about literally 50 pages of data for each hospital, which actually then you can drill down in. It’s all available online, but only obviously to the hospital that actually need to access it, so it’s not available to external private sector organisations. I think for obvious reasons.
Through actually delving into that model hospital, you can actually also benchmark yourself against comparable organisations. And by that I mean hospitals that have a similar number of beds, similar type of case mix, similar elective activity. Because there’s no point, you know, St George’s Hospital benchmarking them against Edgware General for example, so they’re comparable hospitals. And in fact NHSI who manage, does everyone know NHS Improvement that manage the model hospital, they actually provide you with a list of the hospitals that you are compared to. And all sorts of interesting information can come out of the model hospital. So I think it’s very much worth mentioning that, and I do wonder how far that is going to drill into our services, and that would be something probably to watch out for as well.
I think the other main recommendation that came out of the Carter review was around the future operating model. I don’t know whether there’s anyone here from NHS Supply Chain. But obviously NHS Supply Chain, as we all know and love, have had quite major procurement transformation programme themselves. So now they’re the 11 category towers that cover capital, medical and non-medical spend. Does everyone know about the capital towers? Yeah OK. So capital towers have actually, the idea of those is that NHS will actually put more and more of their spend through the category towers, and obviously NHS Supply Chain are going to save billions of, millions actually, millions of pounds just from that initiative alone.
So the idea is that we flex the buying power of the NHS. And it’s something that probably the NHS has been very bad at in the past. And whether having a transformation programme is going to make that different, it’s quite difficult isn’t it? I mean it’s a sort of unwieldy machine, but we know and love it, and at the end of the day it’s still something that we’re all very proud of, so we need to make it work. So I think a lot of the influences have been around the Lord Carter review and actually making recommendations. One of the big recommendations or one of the big focuses of the Lord Carter review was about workforce, and I think none of you will be surprised to know that workforce is the biggest challenge and the biggest risk to the NHS. Actually not just controlling spend, but also actually recruiting the right number of people and the right skills. And I did promise myself I wasn’t going to mention Brexit during this presentation, because we’re all bored of it, but that actually is something that will really heavily influence the recruitment of future skilled labour and people as well, professionals.
So the other theme that has really been quite important is the 10-year plan. And I’m not going to go into this in too much detail. And I am trying to just set the context. So let’s get on with talking about how this impacts on us. But the NHS 10-year plan does actually look at future funding and actually gives some increases in funding for the NHS. So there are some initiatives and there is some money available to actually invest more in medical equipment, technology, integration etc., and we’ll look at that in a little while.
So, just to summarise, how will this impact the NHS? Well we’ve talked about productivity, efficiency. Integration we’ve talked a lot about. The need to actually have better digital technology, that’s also very important. So genomics is obviously another area. The trends and advances in technology, artificial intelligence. I’m too old to start learning computer science now but I would think one of the things that has come out of this conference is the need to actually upskill and develop clinical engineers with additional skills around being able to actually talk IT language, talk to IT people, which is a good start, and I think that’s obviously something that will be important: the digital age. This is no longer the stuff that science fiction is made of; this is here now. Suppliers are actually building a lot of AI technology into their systems. And obviously while hopefully we’ll never completely replace the human, we won’t be robots; there will be a big change.
So the impact on our profession, which is really the point I wanted to get to slowly, the impact on our profession from the transformation agenda I think there’s a number of areas. Obviously technology, I’m not going to dwell on that because I think enough has been said during the conference about how technology is moving and how we need to move with it. I think geography, I don’t know whether anyone is aware of the sustainability and transformation plans, which means collaboration not competition, so the NHS is very much moving towards collaborating with other organisations, not just NHS hospitals, local councils, to actually improve public health, social care and health care.
So that is actually very important in terms of having an influence on how our services look in the future, you know, does every hospital need its own clinical engineering department, I’m just raising the questions and hopefully provoking some of the thoughts. There needs to be more look at how you collaborate perhaps with neighbouring organisations. And I think that’s something that will increase. I think also more community locations. We’ve gone full circle. I mean when I started in the NHS in ’81 my health authority had about one acute hospital and five community hospitals spread across North London, and they were all closed of course. Now we’re building, continuing to build quite a lot of new community facilities. They’re actually springing up all around us and actually diagnostic centres, large GP practices that now look more like outpatient facilities. So I think there’s a lot of move from shifting something out of a very expensive acute hospital state into the community. So that’s actually going to affect us, because that means we’re going to be looking after probably more assets spread across different geography.
More insourcing versus outsourcing, and I don’t mean we should do more insourcing. So I’m not saying we should get rid of all our private sector contracts, but I think what we need to do is focus on what is the objective of actually insourcing or outsourcing EBME or clinical engineering services? And actually look at, I mean the solution will change depending on sort of local management, leadership etc., but actually there is really nothing that the private sector can do that the public sector can’t do themselves without the right investment and infrastructure.
So I think that’s actually something quite important. And I think that’s actually, I don’t know whether Hasan’s here from Northampton at all? No. So I mean hospitals, it’s unheard of but they’re actually moving some of their services back in-house, because actually they recognise that probably some of the value can be added by having the services in-house. I’m not actually going either way. I’m poacher come gamekeeper as they say. Efficiency, I think you’ve got the general message. I mean transformation can mean doing more for less, doing things differently, but also making sure you’re got control of data and you can use that data to drive some of that efficiency.
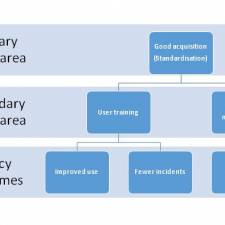
I think our services are typically driven by very competent but very disconnected services. And I don’t know where everyone thinks their organisation might be on this journey, but in my experience of doing a lot of consultancy over the last few years, medical device consultancy, there’s certainly, I haven’t really come across anyone that’s actually at the right-hand side of that slide. And so I think we’ve got work to do. And I think that’s the message there. We need to have the right systems in place, fully integrated systems, be engaging with stakeholders, IT, finance, procurement. Does anyone, well we’re going to talk about that probably in the discussion so.
I just want to just mention a case study, which is some work that we did with Royal Surrey. The main purpose of actually mentioning this is more to support the move to different models of delivering our services. So Royal Surrey Hospital actually commissioned NTS to undertake a full hospital equipment audit, where we probably found far more than 600 items that they didn’t know about, it was something like 3,000 out of 10,000 items, but equally the IBME system had 6,000 items that just didn’t exist. So there is a need to not just look at new equipment going onto the database but clearly make sure you’ve got a system in place for tracking stuff that’s going off.
So that hospital has now set up a wholly owned subsidiary. I don’t know whether anyone is familiar with this, but this is a limited company wholly owned by the hospital. And the idea is that they are delivering their own managed equipment service within the subsidiary. So they are, they’ve tuped over the EBME staff, the radiotherapy technical team, and they’re actually delivering their own services, and actually achieving some of the VAT and tax and efficiency savings that you would if you were outsourcing the managed equipment service. So that’s the sort of, you know, a trend as it were that may, it has actually been recently I think deemed that every single hospital trying to set up one of these vehicles does need to have approval from NHS Improvement; whereas before foundation trusts could just do them themselves.
So Royal Surrey Hospital, we’ve actually got a proper case study on our stand. So if you want to pick up a copy of that feel free to pop by. I haven’t put too much detail but the whole idea is the sort of, C22, Ruth, I think, C22, yeah. The whole point about the model is actually something that we advocate whether this is an outsourced subsidiary or anything else, and that is really to make sure that all the actual, I can’t work this anyway, let me see, so this whole sort of function, which is the medical device management function that we all know and love, this is actually delivered in a very joined-up way rather than a siloed way. And I think that can be achieved whether it’s a subsidiary or whether it’s a hospital or whether it’s a private, as we’ve heard, that can also be achieved whether it’s an outsourced contract as well, as we heard at Royal National Orthopaedic.
So the transformation journey, we need to help in this journey. I mean we’re not going to be able to achieve what the NHS plan visions or Lord Carter visions on our own, but we’re a contributor. And I think that that is actually the message that I want to try to get over. So we need to actually help our organisations understand where value is and where it drains away. We need to look at improvements in the way that we handle data. And I don’t mean just data for the equipment you look after; we should be looking after all equipment across the organisation. Whether it’s imaging, pathology, electro-medical, we need, you don’t have to fix an MRI scanner, but actually you need to know when it has been fixed and when it should be maintained, and all of that should be on a central database. We need to get better control, better people management, better value management, better compliance, you know, better everything. Maybe I’m being a bit optimistic about how we can just contribute to that but, you know, if you’re not in the game you can’t actually make a difference, and that’s actually the message.
So, the drivers, I think again through the conference we’ve heard a lot about governance, top of the agenda. No argument from me that governance is the most important area. But obviously that has to be delivered, under the constraints of the NHS funding regime, it needs to be delivered in a way that we actually embrace and harness all the resources that are available. Reducing cost of ownership, that is something that we are very much in control of, too much decision making by users means that actually money just leaks out of the system. Because they’ve done something the same way the whole time they want to carry on that way, we can actually influence them, coax them. We can’t force them but we can coax them, work with them, build trust and relationships to actually make them listen. And that’s not just the clinical stakeholders; that’s your chief exec, your finance director. And if you don’t know them personally you need to go and knock on their door and introduce yourself, because actually you’re very important to what they’re trying to deliver.
So, the whole managing the equipment lifecycle, this is where we really have our strength. We know about the equipment onsite. We probably know more than any other single person in the hospital where equipment is, what its problems are, when it needs to be replaced; we just need to be better at actually putting that into a plan. So putting it into a lifecycle management plan, a replacement plan and looking at actually bringing in and presenting information to the people that make the decisions, to the people that have to write the business cases with your help, the people that have to present to trust board or go to NHSI with their begging bowl. We need to manage obviously suppliers as well, compliance and performance, and make sure that actually you’re getting out of your suppliers what you’re paying for. And that is actually, it’s no laughing matter that actually equipment that you’re paying fully comprehensive service contracts on, some of it sometimes isn’t even maintained over the course of a year or two years, or sometimes worse.
So I think we internationally have accepted that technology is actually an accelerant for transformation. Well I’d just like to put to you that actually you’re in charge of the technology within your organisations. You can do some of the future horizon scanning. You can help the clinical stakeholders, the finance, the procurement, the IT people to actually understand what technology looks like and how actually that can help to deliver some of the savings. Our profession needs to support that agenda wholeheartedly and I’m very passionate about that.
So finally some considerations for you, the audience, for when you go back after this lovely conference, go back and think about how you can actually contribute to your organisations. Is there potential for you to improve governance? What are the benefits that you can actually add to the process? How can you help make the most of technology? How can you identify for example what is needed? Even if the funding isn’t immediately available, you know, put a five-year plan together. Take it to your ops director, finance director, estates director, whoever. Can you reduce costs and help improve value? And I’ll just leave you with some of those sort of thoughts really that how do you feel you can actually make a difference? And finally if you think I’m being too optimistic, and hopefully this isn’t your trust board or actually your medical devices group or committee, what if we don’t change at all and just something magical happens? Thank you.
Caroline Finlay's presentation at the EBME Expo Innovation in procurement and the transformation agenda